Learn Everything About Stem Cells – In Simple Terms
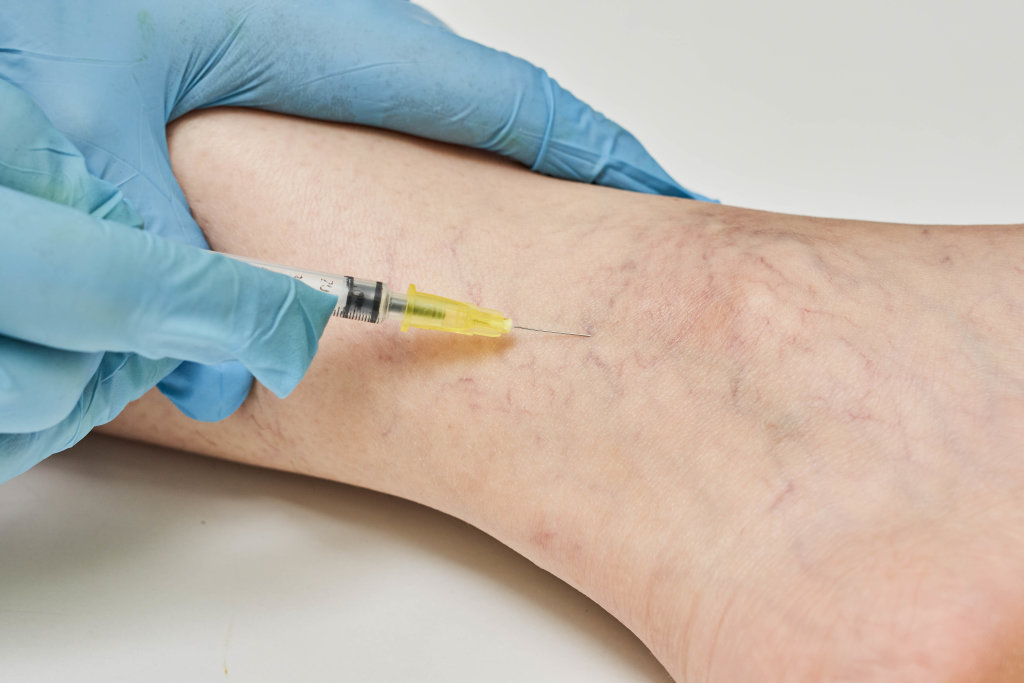
Spider veins are those little bothersome blue, red, or purple veins that seem to develop in patches. Most spider veins occur on the legs. Although they are not a functional problem in and of themselves, they are the physical signs of a problem with the larger veins that control blood flow from the legs back to the heart.
The larger veins in the legs contain one-way valves. Muscle action in the legs pushes the low-pressure blood flow through the venous system upwards and the valves keep the blood from pooling. Over time, these valves become incompetent and the blood backs up from the deep veins to the more superficial veins, causing spider veins to develop. The problem is more common in women particularly those who have had children, in obese patients, and patients that have jobs where they do a lot of standing such as teachers, waiters, nurses, and even surgeons.
Once spider veins develop, the evaluation and treatment must determine whether there is a significant problem with the deeper system, that needs to be treated first. This includes varicose veins and obstruction of the saphenous vein system. Noninvasive studies including Doppler studies will help diagnose these problems. If a larger problem exists, the physician must treat this first, by either ligating the veins, which means tying them off, or using a laser placed inside the vein to obliterate it.
The spider veins the most common treatment is sclerotherapy. This is a procedure where an irritant such as high concentrations of saline solution or a detergent is injected into the vein with a very small needle, to cause damage to the wall of the vein and obliterate it. If the vein is too small to insert a needle into, the laser has been shown to be effective.
With either treatment, it is often necessary to treat a second or third time in the area where the spider veins are. Wearing a support hose helps to improve the tone of the legs and decrease the development of spider veins, but it’s difficult to wear a support hose in warm climates such as Houston. Elevating the legs during the day for even 15 minutes will also help with the problem. People that sit on cramped trains or planes for hours should get up every so often and stand on their toes and move the seat back and forth to help push blood through the system.